Is anyone else irritated by medical insurance companies’ efforts to improve the health of their members by encouraging them to do recommended tests based on claims-made data? Recently, a patient asked me if he should get the pulmonary function tests his insurance company recommended based on his asthma diagnosis. He does have mild intermittent asthma. He uses a steroid inhaler once a year during the spring for about a month and might use his rescue inhaler with exercise four or five other times during the year.
Is anyone else irritated by medical insurance companies’ efforts to improve the health of their members by encouraging them to do recommended tests based on claims-made data? Recently, a patient asked me if he should get the pulmonary function tests his insurance company recommended based on his asthma diagnosis. He does have mild intermittent asthma. He uses a steroid inhaler once a year during the spring for about a month and might use his rescue inhaler with exercise four or five other times during the year. If you check the guidelines put out by the National Asthma Education and Prevention Program it is recommended that a spirometry test or PFTs be performed annually to assess any changes in lung function. The fact is, this patient has been treating his asthma the same way for about fifteen years. He feels fine. So will doing PFTs make a difference? We discussed it (over Christmas and through the patient portal, which I love) and decided that doing testing was unlikely to cause a change in therapy. Since he had better things to do than PFTs he would prefer to skip the tests. Hopefully he won’t see an increase in his premium for refusing to follow his insurance company’s medical advice. Does this make me worry about becoming nothing more than a flunky ordering tests for patients based on Humana or Aetna or Anthem’s “best practices”? In a word, yes.
What irritates me more, is being faxed long lists of patient names with recommendations for mammograms, colonoscopies or diabetic eye exams. Our office is supposed to pull those charts and encourage patients to have their preventive exams. Of course if we do pull them, it turns out the “claims-made” data from the insurance company isn’t all that accurate and many patients have already had their tests done. Thus another waste of the office employees’ time pulling charts. Hopefully it will be easier with electronic records.
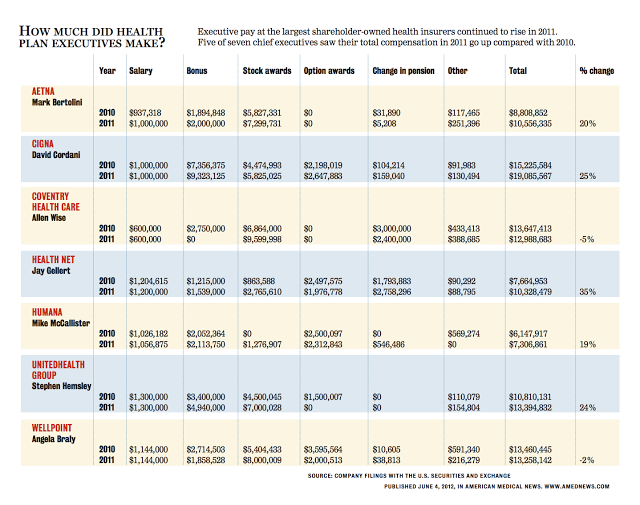
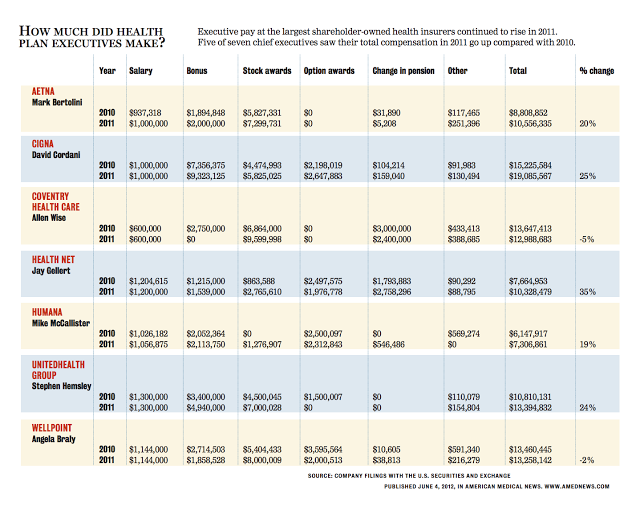
When I want medical advice I will talk to my doctor or find an expert on-line, I will not talk to my insurance company. I do not want or need coupons from Humana. Nor do I want my insurance company to remind me of preventive care visits via my telephone. My patients are thrilled by it, however. “Humana pays for me to go to Silver Sneakers! Isn’t that great?” or “A free 30-day Jenny Craig membership is available, what do you think doc?”
Just call me Thomas, because I am a doubter. Nothing is truly free in the insurance business, so somewhere along the line the consumer is paying for the SilverSneaker membership and the salary of the individual who is soliciting companies to provide coupons from the insurance company. Please, just pay my claims and not give me such a headache trying to obtain my prescription from your 90 day pharmacy service. That’s what I would call good service!